Disease
Idiopathic retinal vasculitis, aneurysms, and neuroretinitis (IRVAN) syndrome is a rare clinical entity of unknown etiology.
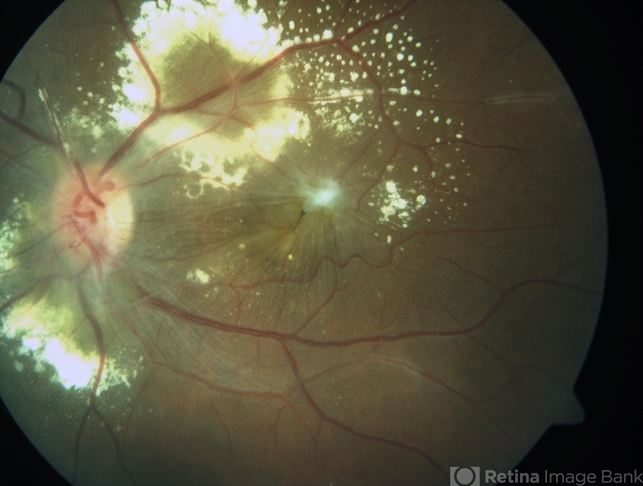
Some authors have speculated an association between positive P-ANCA s (Perinuclear AntiNeutrophil Cytoplasmic Antibodies) systemic vasculitis and antiphospholipid syndrome.
Stages
- Stage 1: Macroaneurysms, exudation, neuroretinitis, retinal vasculitis.
- Stage 2: Capillary nonperfusion (angiographic evidence)
- Stage 3: Posterior segment neovascularization of disc or elsewhere and/or vitreous hemorrhage.
- Stage 4 : Anterior segment neovascularization (rubeosis iridis)
- Stage 5 : Neovascular glaucoma.
Diagnosis
The diagnosis of Idiopathic retinal vasculitis, aneurysms, and neuroretinitis (IRVAN) is based on a constellation of clinical features.
Three major criteria (retinal vasculitis, aneurysmal dilations at arterial bifurcations, and neuroretinitis) and 3 minor criteria (peripheral capillary nonperfusion, retinal neovascularization, and macular exudation) are used to diagnose IRVAN.
Patients with IRVAN usually present with decreased visual acuity in one or both eyes. They may have a variable number of cells in the anterior chamber and the vitreous.
The retinal arterioles have multiple aneurysmal dilatations extending through the first several orders of arterial branching until mid-periphery.
The aneurysms are commonly found on the optic nerve, a site where typical senile retinal macroaneurysms are not. The aneurysms are typically found at branching points of the arteries, and may be fusiform, Y-shaped, or spheroid in shape.
In segments between the aneurysms the retinal arteries frequently show marked caliber variations. Arterial aneurysms clinically resemble multiple and consecutive “knots of a cord”.
Disc neovascularization may be observed in severe and advanced cases of IRVAN, with peripheral capillary dropout. Vitreous hemorrhage can result from retinal neovascularization.
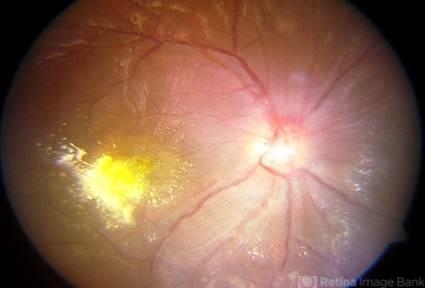
Non-complicated cases may have a slight swelling of the optic nerve head, highlighted in the late phases of fluorescein angiography.
Some authors think there are no true neuroretinitis, leakage occurs from the aneurysms on the optic nerve head, and periarterial lipid exudation results from retinal artery aneurysms.
Retinal vascular sheathing may occur, but it is not a prominent feature of the disorder in most patients. In the retinal periphery, there is a variable amount of retinal nonperfusion, with obliteration of the arteries, veins, and retinal capillaries.
In the perfused area bordering the peripheral areas of nonperfusion, the retinal veins may show abnormal caliber alterations.
If the ischemic load of the nonperfused retina reaches a critical level, retinal and iris neovascularization may develop. Interestingly, neo-vessels may sometimes reproduce arterial macroaneurysms seen in the retinal vasculature ( Richard F Spaide MD, personal communication ).
In severely affected individuals, vitreous hemorrhage and neovascular glaucoma have developed.
Although lipid deposition is not common in most patients with uveitis, patients with IRVAN frequently have marked intraretinal lipid deposition.
This lipid is usually found in the peripapillary region and may extend into the macula leaving a macular star or massive lipid accumulation.
The lipid is generally found near the greatest concentration of aneurysms ( peripapillary location and along the arcades ).
The retina in these areas is commonly edematous and may be detached by exudative fluid. As time goes by, a fibrous grayish macular scar may develop as a legacy of long-standing exudation in the macula.
Signs
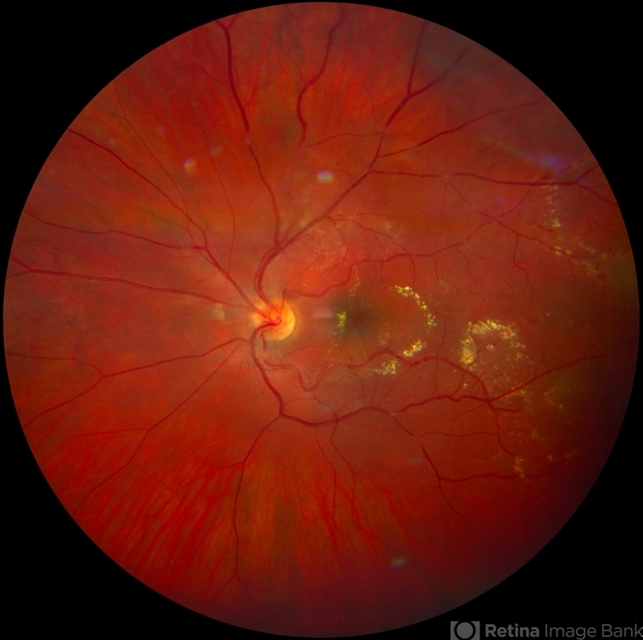
- Multiple post-equatorial arterial aneurysms in the retina and optic disc head.
- Peripapillary lipid exudation associated with macroaneurysms and retinal vasculitis.
- Retinal hemorrhages in the posterior pole.
- Peripheral capillary nonperfusion
- Retinal vascular sheathing
- Swelling of the optic nerve
- Retinal neovascularization
- Optic disc neovascularization
Symptoms
Asymptomatic
Patients may not complain about loss of vision in spite of having a severe disease if it does not affect the macula at the initial presentation.
Nonspecific symptoms
For instance, multiple visits for a change of glasses due to blurred vision.
Clinical diagnosis
Patients with Idiopathic retinal vasculitis, aneurysms, and neuroretinitis (IRVAN) are, sometimes, over-investigated for systemic causes of retinal disease.
However, IRVAN seems to produce only ophthalmic manifestations, with general workup being mostly unremarkable.
Retinal imaging is a key element for a rapid diagnosis of IRVAN, and a multimodal imaging approach is recommended when this syndrome is suspected, to collect all possible diagnostic criteria.
Dye-mediated angiographies ( fluorescein and indocyanine green) remain the standard imaging modalities for confirming the clinical diagnosis of IRVAN.
Would you have interest in taking retinal images with your smartphone?
Fundus photography is superior to fundus analysis as it enables intraocular pathologies to be photo-captured and encrypted information to be shared with colleagues and patients.
Recent technologies allow smartphone-based attachments and integrated lens adaptors to transform the smartphone into a portable fundus camera and Retinal imaging by smartphone.
RETINAL IMAGING BY YOUR SMARTPHONE
REFERENCES
- Chang TS, Aylward GW, Davis JL, et al. Idiopathic retinal vasculitis, aneurysms, and neuro-retinitis. Ophthalmology. 1995;102:1089–1097.
- Samuel MA, Equi RA, Chang TS, et al. Idiopathic retinitis, vasculitis, aneurysms, and neuroretinitis (IRVAN): new observations and a proposed staging system. Ophthalmology. 2007;114:1526–1529.
- Centers for Disease Control (CDC). International Classification of Diseases, Tenth Revision, Clinical Modification(ICD-10-CM): FY 2017 version; 2017. Available at: https://www.cdc.gov/nchs/icd/icd10cm.htm. Accessed November 23,2017.
- Flynn J, Clarkson J, Curtin V, Flynn Jr. H, Hurtes R, Smith J. J. Donald M Gass, MD : Festschrift Editorial. Am J Ophthalmol 2004;137,3:480-2.
- Gass JD. Stereoscopic Atlas of Macular Diseases: Diagnosis and Treatment. 3rd ed. St Louis: Mosby; 1987.
RETINAL IMAGING BY YOUR SMARTPHONE

RETINAL IMAGING BY YOUR SMARTPHONE

