CASE REPORT
A 34-year-old female presented with a six-month history of persistent eye redness and discomfort in both eyes, denying any significant ocular trauma, prior eye conditions, allergies, or systemic diseases, with no recent eye surgeries or procedures.
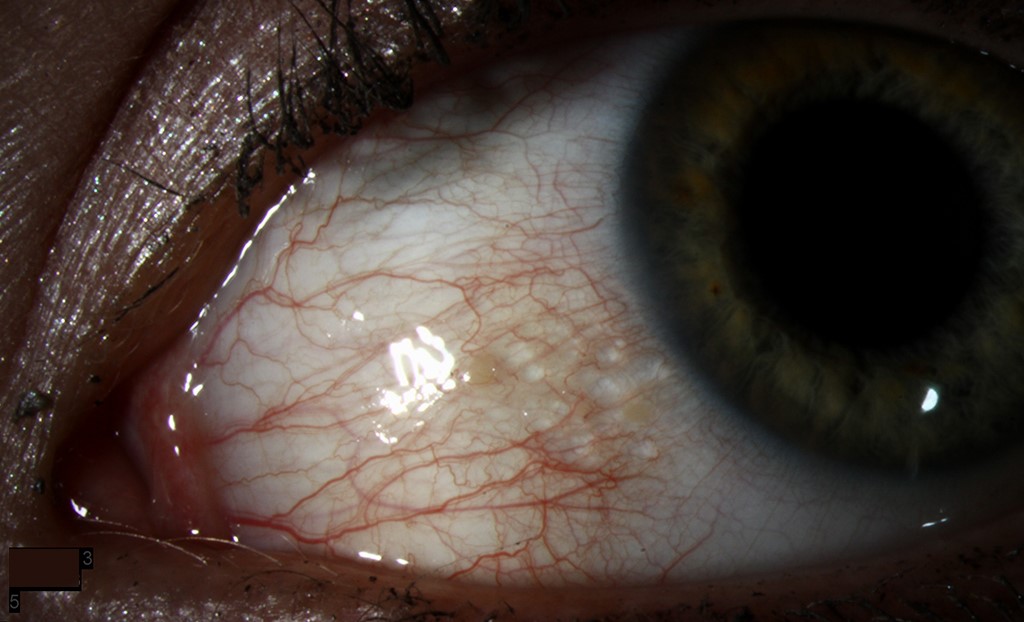
Presenting Symptoms included bilateral eye redness that did not improve with over-the-counter artificial tears, a constant foreign body sensation causing discomfort, and intermittent blurred vision, particularly in the morning.
Clinical Examination findings revealed 20/20 visual acuity in both eyes, normal external eye appearance with no swelling, ptosis, or proptosis, and a close slit-lamp examination demonstrated the presence of multiple translucent and dilated lymphatic vessels, predominantly in the upper temporal bulbar conjunctiva of both eyes.
The tear film and corneal surfaces appeared healthy with no signs of dry eye disease or corneal involvement, and pupils were equal in size and reacted briskly to light.
Diagnostic tests included negative fluorescein staining for corneal abrasions, Schirmer’s test results indicating normal tear production, and a confirmed diagnosis of conjunctival lymphangiectasia through a conjunctival biopsy.
DISEASE
Conjunctival lymphangiectasia is a rare condition characterized by dilated lymphatic vessels in the conjunctiva, the thin, transparent membrane that covers the front surface of the eye and lines the inside of the eyelids.
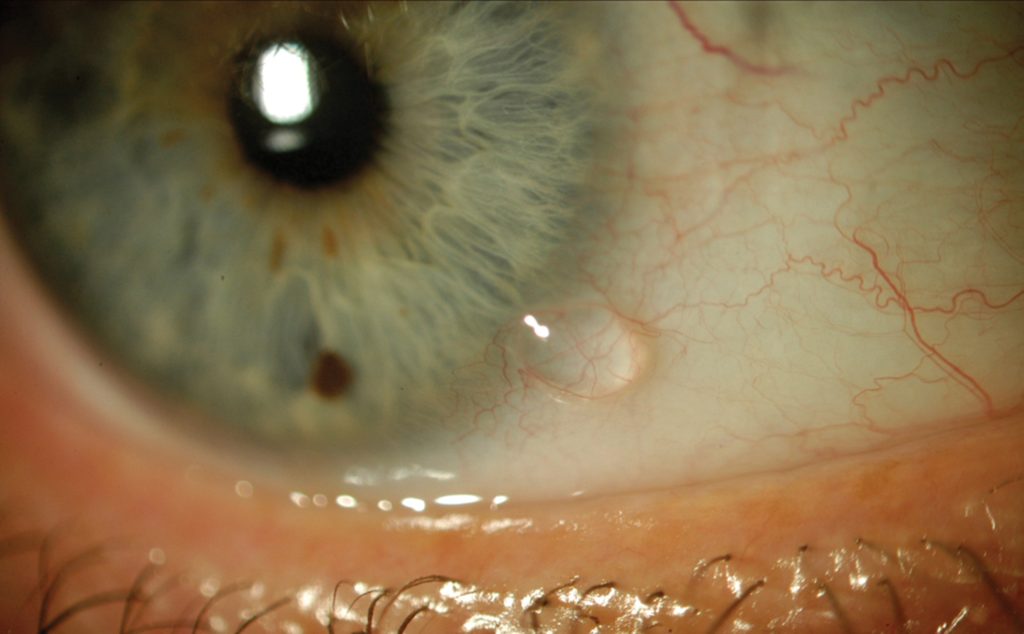
The lymphatic vessels in the conjunctiva are responsible for draining excess fluid and waste products from the eye, and their dilation can lead to a range of symptoms, including redness, swelling, irritation, and tearing.
Conjunctival Lymphangiectasia can manifest in two distinct forms: diffuse or localized. In the diffuse form, there is swelling of the conjunctiva (chemosis), and the lymphatic vessels are spread out over a wide area.
In the localized form, the lymphatic vessels appear as a series of small, pearl-like bumps (referred to as a “string of pearls” appearance).
This localized form may be present in only one or both eyes, which is more commonly associated with a systemic disease.
Lymphangiectasia hemorrhagic conjunctivae is the term used to describe a lesion that occurs when there is a link between a blood vessel and the enlarged lymphatics, causing the area to intermittently fill with blood.
Diagnosis
Diagnosis typically involves a detailed eye examination, as well as imaging tests such as ultrasound or anterior segment optical coherence tomography (ASOCT), to evaluate the extent of lymphatic dilation.
The hyporeflective lesions vary in size and are cyst-like lesions on ASOCT. Histopathological examination is invasive and confirms the diagnosis.
MANAGEMENT
In most cases, conjunctival lymphangiectasia resolves on its own without any intervention.
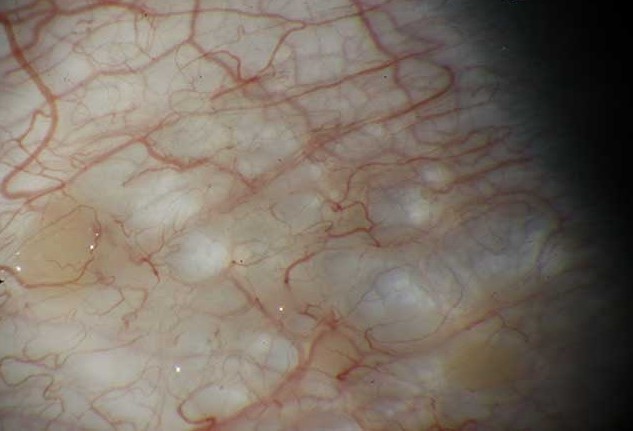
Treatment options for conjunctival lymphangiectasia depend on the severity of the symptoms. They may include topical antihistamines and steroids or oral medications to reduce inflammation and swelling and surgical intervention in more severe cases.
Patients with conjunctival lymphangiectasia have several treatment options available, including surgical excision, cryotherapy, anti-vascular endothelial growth factor (anti-VEGF) subconjunctival injections, and radiowave electro-ablation.
Welch et al. described a successful treatment approach involving excision followed by conjunctival autograft or amniotic membrane transplant, resulting in reduced recurrence rates.
A case report published in 2018 presented the option of lesion resection followed by suturing the remaining tissue with an 8.0 Vicryl.
Liquid nitrogen cryotherapy, which was described in a 2009 article, can be an efficient surgical alternative for the management of conjunctival lymphangiectasia. In certain cases, cryotherapy may need to be repeated to achieve optimal results.
A single dose of subconjunctival injection with Avastin has also been effective in targeting VEGF, which plays a significant role in lymphangiogenesis.
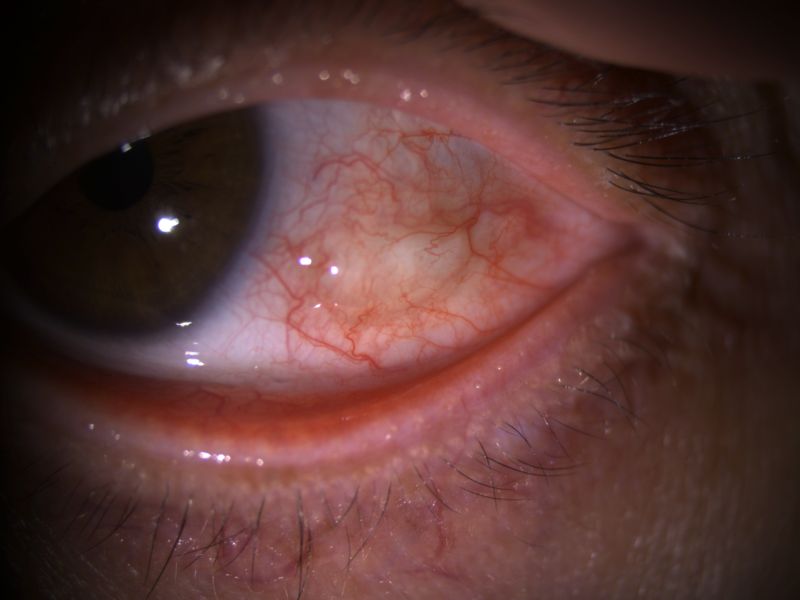
The latest approach for treating conjunctival lymphangiectasia involves using high-frequency radiowaves to ablate the affected area. This technique is highly promising, as it helps retain more conjunctival tissue than surgical excision.
It is also a preferred first-line treatment option for conjunctival lymphangiectasia. While surgical excision is a more invasive option, it is associated with a much lower recurrence rate than other treatment modalities.
HOW TO TAKE SLIT-LAMP EXAM IMAGES WITH A SMARTPHONE?
Smartphone slit-lamp photography is a new advancement in the field of science and technology in which photographs of the desired slit-lamp finding can be taken with smartphones by using the slit-lamp adapters.
Slit-lamp Smartphone photography
REFERENCES
- Cristea, A.P., L.T. Petrescu, and C. Stan, Conjunctival Lymphangiectasia – case report. Rom J Ophthalmol, 2022. 66(4): p. 365-368.
- Awdry, P., Lymphangiectasia hemorrhagica conjunctivae. Br J Ophthalmol, 1969. 53(4): p. 274-8.
- Welch, J., et al., Conjunctival lymphangiectasia: a report of 11 cases and review of literature. Surv Ophthalmol, 2012. 57(2): p. 136-48.
- Perry, H.D. and A.J. Cossari, Chronic lymphangiectasis in Turner’s syndrome. Br J Ophthalmol, 1986. 70(5): p. 396-9.
- Ramasubramanian, A., et al., Conjunctival edema and distichiasis in association with congenital lymphedema of the lower legs. Ophthalmic Plast Reconstr Surg, 2009. 25(2): p. 148-50.
- Tabbara, K.F. and S.A. Baghdassarian, Chronic hereditary lymphedema of the legs with congenital conjunctival lymphedema. Am J Ophthalmol, 1972. 73(4): p. 531-2.
Slit-lamp Smartphone photography

RETINAL IMAGING BY YOUR SMARTPHONE

