CASE REPORT
A 28-year-old lady presented with acute vision loss in the right eye for 3 days. The left eye examination was unremarkable. Best-corrected visual acuity in the right eye was 20/40. Anterior segment examination revealed a clear lens with no evidence of inflammation. There were no vitreous cells.
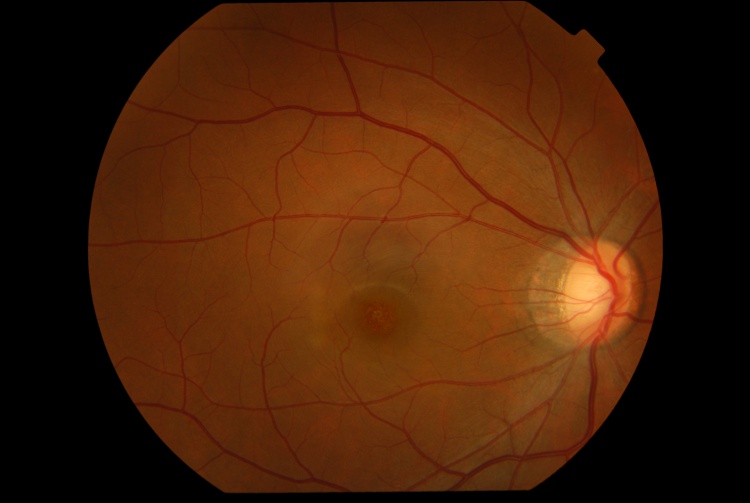
Fundus examination of the right eye revealed a round orange lesion surrounded by a hypopigmented halo in the fovea with multiple tiny hypopigmented lesions temporal to the fovea.
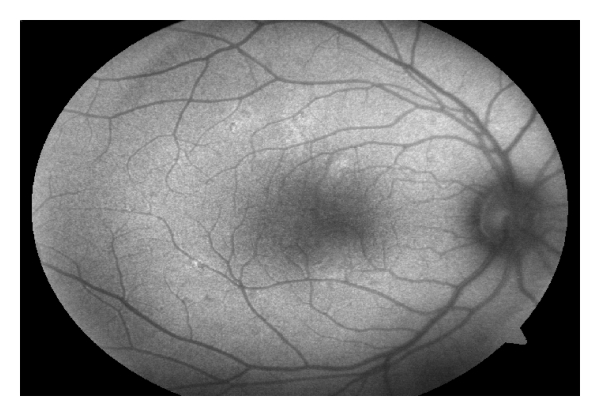
Fundus autofluorescence imaging of the right eye showed hyper-autofluorescent lesions temporal to the fovea corresponding to the hypopigmented lesions seen temporal to the fovea.
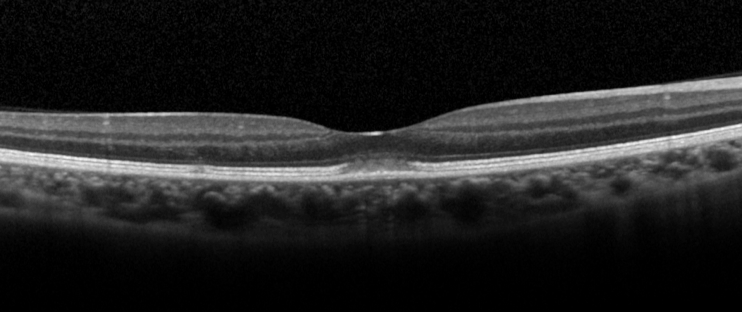
Spectral-domain optical coherence tomography of the right eye revealed a subfoveal hyperreflective lesion in the outer retina with disruption of the ellipsoid zone and interdigitation zone with a linear extension upward.
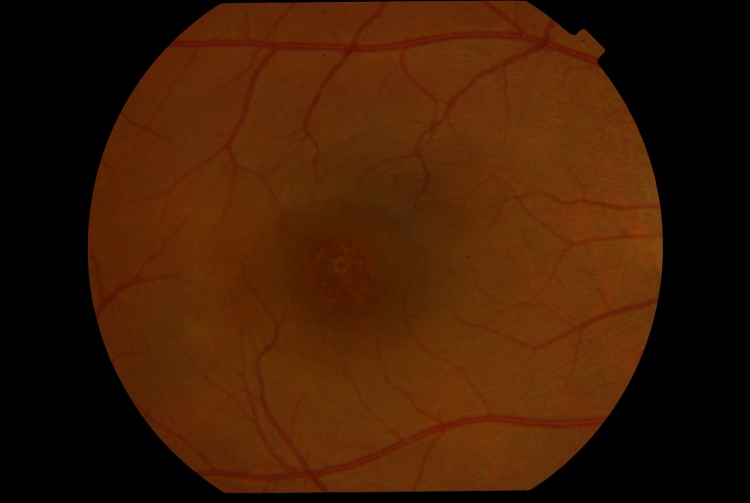
A multicolor composite image of the right eye revealed the foveal lesion as a circular red patch with an inferior orange extension. The infrared reflectance image revealed a hyperreflective area corresponding to the foveal lesion.
The blue and green reflectance images were unremarkable. A diagnosis of Acute Retinal Pigment Epitheliitis (ARPE) was made based on history, clinical and imaging findings.
Acute Retinal Pigment Epitheliitis (ARPE) DISEASE entity
Acute Retinal Pigment Epitheliitis (ARPE), also known as Krill’s disease is a rare, idiopathic, self-limiting inflammatory disease of the retina that commonly affects young adults. It was first described by Alex E. Krill and August F. Deutman in six patients in 1972.
These six patients, consisting of three males and three females, were of the ages of 16, 18, 22, 43, 45, and 46 years. Krill and Deutman described the retinal lesions to be clusters of small round, dark gray spots surrounded by circular whitish depigmented zones located in the macula.
The condition had an acute onset with fairly rapid resolution in 6 to 12 weeks, and recovery to normal or almost normal vision was achieved in all six patients.
Although in previous studies, it was believed that the primary site of inflammation was located at the retinal pigment epithelium (RPE), recent studies using spectral-domain optical coherence tomography suggested the primary site of inflammation is located at the interdigitation zone i.e. the contact between photoreceptors and RPE instead of the RPE itself.
Acute Retinal Pigment Epitheliitis (ARPE) typically affects young healthy adults between the age of 20 and 50 years. It is rare and the incidence is unknown. Males and females are equally likely to be affected. In a case series of 18 patients in South Korea, the male-to-female ratio was 6:4. No racial predisposition has been described.
The etiology and pathophysiology are unknown. Similar to many white dot syndromes, flu-like symptoms have been reported to occur before the onset of ARPE, suggesting viral infection may play a role in the pathogenesis.
However, a case series of 18 patients showed that only 17% of patients had prodromal influenza-like symptoms before the onset of the disease.
Acute Retinal Pigment Epitheliitis (ARPE) MANAGEMENT
General treatment
No treatment is necessary because of the self-limiting nature of the disease. Spontaneous resolution of the lesion and recovery of vision occurs in all patients without treatment.
The use of oral steroids does not shorten the course of recovery. In a case series of 4 patients with ARPE, the 3 patients who were treated with oral steroids had slower recovery of vision than the patient without any treatment.
Medical follow up
Patients should be followed with serial visual acuity tests, fundal examinations, and OCT. Complete recovery of visual acuity, fundal abnormalities, and OCT retinal bands is expected within weeks.
During recovery, OCT shows a typical pattern where the inflammatory lesion reduces in height and the retinal layers restore in order from inner to outer layers. The recovery involves a sequence of:
(1) a decrease in height of OCT hyper-reflective lesion and the displaced external limiting membrane returned to its normal position with irregularity.
(2) complete disappearance of the hyper-reflective lesion.
(3) restoration of the external limiting membrane.
(4) restoration of the ellipsoid zone.
(5) restoration of the interdigitation zone. Occasionally, there is a persistent defect in the OCT ellipsoid zone associated with incomplete visual recovery.
Prognosis
The prognosis is excellent. Complete recovery of visual acuity to 20/20 occurred in 89% of patients within 2 months.
However, incomplete visual recovery for more than 1 year has been described. Poor prognostic factors included poor baseline visual acuity of <20/70 and extensive retinal involvement involving the outer nuclear layer. Recurrences are exceedingly rare.
Would you have interest in taking retinal images with your smartphone?
Fundus photography is superior to fundus analysis as it enables intraocular pathologies to be photo-captured and encrypted information to be shared with colleagues and patients.
Recent technologies allow smartphone-based attachments and integrated lens adaptors to transform the smartphone into a portable fundus camera and Retinal imaging by smartphone.
RETINAL IMAGING BY YOUR SMARTPHONE
REFERENCES
- Cho HJ, Han SY, Cho SW, Lee DW, Lee TG, Kim CG, Kim JW. Acute retinal pigment epitheliitis: spectral-domain optical coherence tomography findings in 18 cases. Invest Ophthalmol Vis Sci 2014;55(5):3314-9.
- Baillif S, Wolff B, Paoli V, Gastaud P, Mauget-Faysse M. Retinal fluorescein and indocyanine green angiography and spectral-domain optical coherence tomography findings in acute retinal pigment epitheliitis. Retina 2011;31(6):1156-63.
- Krill AE, Deutman AF. Acute retinal pigment epitheliitus. Am J Ophthalmol. 1972;74:193-205.
- Iu LPL, Lee R, Fan MCY, Lam WC, Chang RT, Wong IYH. Serial Spectral-Domain Optical Coherence Tomography Findings in Acute Retinal Pigment Epitheliitis and the Correlation to Visual Acuity. Ophthalmology 2017;124(6):903-9.
- De Bats F, Wolff B, Mauget-Faysse M, Scemama C, Kodjikian L. B-scan and “en-face” spectral-domain optical coherence tomography imaging for the diagnosis and follow-up of acute retinal pigment epitheliitis. Case Rep Med 2013;2013:260237.
RETINAL IMAGING BY YOUR SMARTPHONE

RETINAL IMAGING BY YOUR SMARTPHONE

